Dropping your pet off for an anesthetic procedure is one of the most stressful parts of being a pet parent. It is normal to worry about your pet and wonder what they are experiencing at the veterinary clinic. At All Ears Veterinary, we pride ourselves on high-quality medical care that greatly reduces anesthetic risk. From setting up your fur baby’s procedure to providing discharge instructions, we aim to make the experience as safe and smooth as possible.
Prior to Drop-Off

When a pet is scheduled for an anesthetic procedure, a comprehensive plan is always made ahead of time. The first step is for a veterinarian to review the patient’s chart and ensure that there are no health issues precluding anesthesia. This means reviewing their recent physical exams, lab results, and medications.
We then select the appropriate combination and dosages of antibiotics, pain medications, and sedatives. Based on the individual patient, additional medications such as anti-nausea drugs, antacids, or steroids may also be selected. An appropriate rate of intravenous fluids to maintain hydration and blood pressure is also calculated.
We also create tailored emergency protocols for the individual pet, so that we will know what steps to take if there are any issues under anesthesia. These can include drug reversal agents and medication to raise blood pressure.
Prior to Anesthesia
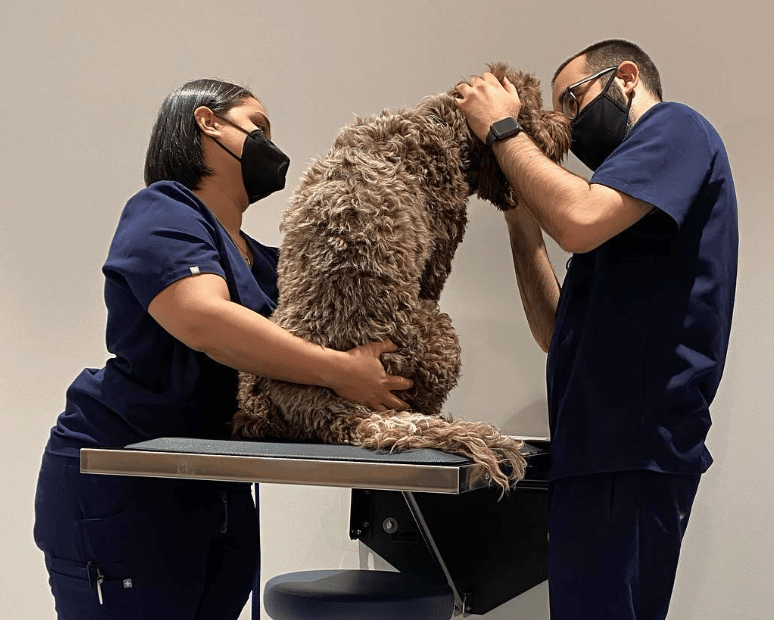
Once a pet is dropped off, the veterinarian performs a physical examination to ensure that the patient is healthy enough for anesthesia. This involves listening to the heart for abnormal sounds, checking their vitals, and ensuring that no new problems have popped up since their last physical. The previously made anesthetic plan is reviewed and all drug dosages are double checked to ensure that your pet is receiving the appropriate treatments.
During this time, all of our equipment is inspected to ensure that there are no mechanical issues. This involves checking that our anesthetic monitoring devices are functioning, that there are no leaks with the anesthesia machine, that the fluid pumps run, and our heating blankets work. We always want to be aware of any potential problems before a pet is hooked up to a machine. In the event that any issues are found, we always have spare equipment.
The next step is placing an intravenous (IV) catheter in one of the pet’s limbs. This gives us quick and easy access to a vein so we can administer all needed medications. The patient is then usually given what are called “premedications.” These are sedatives which relax your pet and lower the amount of inhaled anesthetic gas that they will need.
Monitoring Anesthesia

Your pet is then given a strong sedative to transition them into full anesthesia. Most procedures involve intubating our patients. This means that an endotracheal tube is passed through their throat and hooked up to our anesthesia machine. This allows us to measure the quality of their breaths and breathe for them if needed.
The major benefit of anesthesia is that pets do not perceive pain and have no memory of a highly stressful event. However, anesthesia means that most bodily functions are changed. Pets breathe differently, have lower blood pressure, and become colder when anesthetized. To ensure that your pet remains safe, an experienced team member constantly monitors your pet’s vital signs. These are just some of the things that are trained nurses are constantly keeping an eye on:
- Body Temperature: To prevent a low body-temperature, we use medical-grade heating blankets and fluid warmers.
- Blood Oxygen Levels: Just like us, animals’ blood is usually nearly completely saturated with oxygen. If the oxygen levels ever get low, we know to reduce the amount of anesthesia or adjust their endotracheal tube.
- Blood Pressure: Blood pressure is one of the most important values to monitor. Blood pressure will almost always drop under anesthesia. Keeping it above a certain level ensures that all of your pets’ organs are getting an adequate blood supply. If the blood pressure gets too low, we may reduce the anesthesia, increase their fluids, or give certain medications.
- ECG (Electrocardiogram): Each beat of the heart creates an image that our electrocardiogram measures. By evaluating the shape of the heartbeats, we can determine if there are any dangerous arrhythmias.
- Carbon Dioxide: An animal’s lungs have two main jobs: supplying the body with oxygen and removing the carbon dioxide that builds up as waste. By measuring the amount of carbon dioxide in each exhaled breath, we can assess how well the body is generally functioning under anesthesia. If the levels are inappropriate, we may change how often we breathe for a pet or adjust the amount of anesthetic gas they are inhaling.
A Note on Pain

Gone are the days when people believed that pain was necessary to help pets (and people!) recover. Reducing our patients’ pain is a responsibility that we do not take lightly at All Ears. Every patient receives multiple methods of pain control to help provide the least stressful experience possible. While every case is different, we usually try to incorporate the following three types of pain control:
- Opioids: Opioids such as buprenorphine and hydromorphone provide excellent pain control without significant side effects on most organs in the body. Unlike people, pets are not at high risk for drug dependency.
- Non-Steroidal Anti-Inflammatory Drugs (NSAIDs: NSAIDs reduce both pain and inflammation, making them important in nearly all surgeries. NSAIDs have some potential side effects on the liver, kidneys, and gastrointestinal tract. This is one reason why we always perform bloodwork prior to anesthetized procedures. Examples of canine NSAIDs are Carprofen (Rimadyl) and Meloxicam (Metacam).
- Local Anesthesia: Modern-day medicine now focuses on treating pain as close to the source as possible. Most procedures allow for us to administer locally acting pain medication near the surgical site. This includes dental nerve blocks, intra-testicular anesthesia, and infusing an entire abdomen with absorbable painkillers.
Anesthetic Recovery
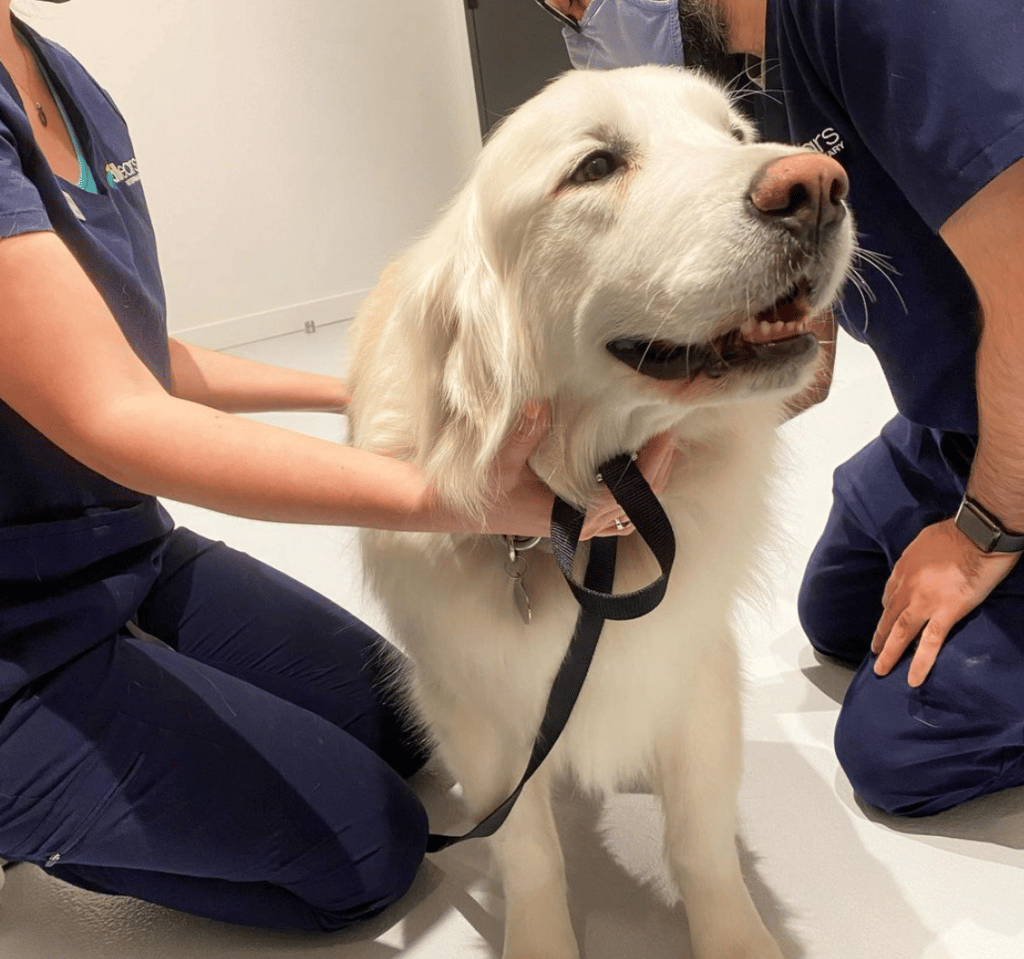
When a pet’s procedure is done, we continue to monitor them closely. Once they are awake enough to swallow on their own, we remove their endotracheal tube and check their vitals for another several minutes. At this point a pet is generally stable enough to continue recovering on their own with us checking in on them as needed, although if there were any concerning signs under anesthesia a pet will be monitored until those signs normalize. All pets are kept in an easily visible location so that we can keep a general eye on them until they are discharged.
At this time the veterinarian will call the pet parent to discuss the procedure and general discharge instructions. We will set up a pick-up time, usually several hours after a procedure has ended. This is to ensure that the pet has enough time to be watched and fully recover.
Surgical Discharge

All pet parents are given an emailed set of discharge instructions. When a pet parent comes to pick up their pet, our nurses go over these instructions. They also discuss how to give any medications and when to start them. We instruct most surgical patients to come back for a free recheck in 10-14 days, though this may vary depending on the procedure that was done.
Do you feel more informed about the process of surgery day? Let us know your thoughts or any questions in the comments below.





Conversation